HEDIS Spotlight: Chlamydia and cervical cancer screenings
HEDIS stands for Healthcare Effectiveness Data and Information Set. It is a widely used set of performance measures by the nation’s health plans, and an essential tool in ensuring that our members are getting the best healthcare possible. It is extremely important that our providers understand the HEDIS® specifications and guidelines. In this section of The Checkup we will highlight different HEDIS metrics. We will provide a description of the measures, the correct billing codes to support services rendered, and tips that include specific resources and tools available to you that correspond with that measure.
MEASURE: Chlamydia Screening
MEASURE DESCRIPTION: Measures the percentage of women 16-24 years of age who were identified as sexually active and who had at least one chlamydia test during the measurement year. “Sexually active” women are identified by those members who were dispensed prescription contraceptives, and/or members who had at least one related encounter with a physician or clinic that may have included pregnancy testing, STD diagnosis, contraceptive services, or history of sexual assault or abuse.
CODING:
Codes to identify chlamydia screening: 87110, 87270, 87320, 87490-87492, 87810
TIPS:
- Remember that chlamydia screening can be performed through a urine test. Offer this as a non-invasive option for your patients.
- Add chlamydia screening as a standard lab for women 16-24 years old. Use well child exams and well women exams for this purpose.
- Perform chlamydia screening every year on every 16-24-year-old female identified as sexually active (use any visit opportunity).
- Perform chlamydia screening on every patient requesting or obtaining contraceptives.
- Ensure that you have an opportunity to speak with your adolescent female patients without her parent.
- Place chlamydia swab next to Pap test or pregnancy detection materials.
MEASURE: Cervical Cancer Screening
MEASURE DESCRIPTION: Measures the percentage of women 21-64 years of age with one or more cervical cytology tests (Pap tests) within the last 3 years or for women 30-64 years of age, a cervical cytology and human papillomavirus (HPV) co-testing within the last 5 years.
EXCLUDES:
- Women who have had a “total”, “complete,” or “radical” vaginal or abdominal hysterectomy or “no residual cervix,” or cervical agenesis or acquired absence of cervix
- Women in hospice
- Female Adolescents ages 16-20 years are not recommended to have a cervical cancer screening unless they have a history of cervical cancer, HIV, or immunodeficiency
CODING:
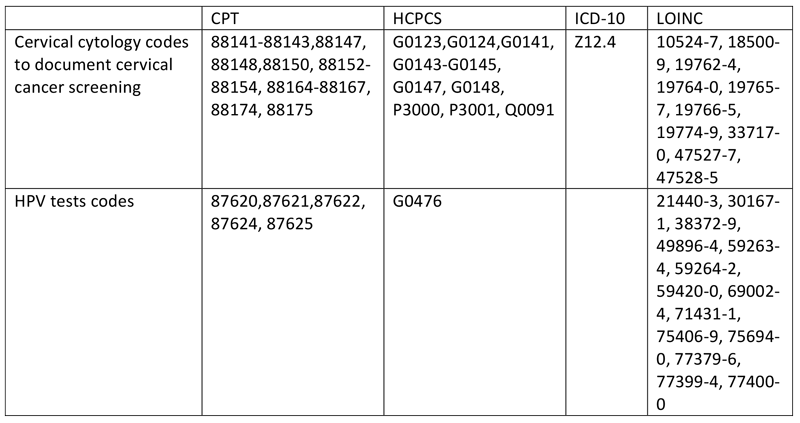
Helpful Tips
- Make sure your medical records reflect:
- The date and type of test that was performed.
- Notes in patient’s chart if patient has a history of hysterectomy and the year it was performed. Include complete details if it was a complete, total, or radical abdominal or vaginal hysterectomy with no residual cervix; also, document history of cervical agenesis or acquired absence of cervix.
- Be a champion in promoting women’s health by reminding them of the importance of annual wellness visits to include Pap tests for all female members ages 21-64 years. Don’t miss opportunities to complete Pap tests during regularly-scheduled well woman visits, sick visits, urine pregnancy tests, UTI, and Chlamydia/STI screening.
- Use a tracking mechanism, (for example, EMR flags and/or manual tracking tool) to identify members due for cervical cancer screening.
- Refer patients to another appropriate provider if your office does not perform Pap tests and request copies of Pap test/HPV co-testing results be sent to your office. Always request records from other providers if the Pap test/HPV contesting has been done elsewhere.
Train your staff on the use of educational materials to promote cervical cancer screening. Display posters/educational messages in treatment rooms and waiting areas to encourage members to initiate discussions with you about screening.






Leave a Reply
You must be logged in to post a comment.