Provider Alert! Second Quarter 2020 HCPCS Updates for Texas Medicaid
Attention: All Providers
Effective Date: July 1, 2020 Updated September 10, 2020
Call to action: Texas Children’s Health Plan (TCHP) aligns with the Healthcare Common Procedure Coding System (HCPCS) additions, revisions, and discontinuations that are implemented for claims processing by TMHP for Texas Medicaid.
How this impacts providers: Second Quarter 2020 HCPCS Added Procedure Codes are as follows:
| Clinician Administered Drug (CAD) Procedure Codes | ||
| C9061 | J0223 | J0691* |
| J0742 | J0791* (replacing C9053) | J0896 |
| J7169* | J7204 | J9177 |
| J9246 | J9358 | Q5119 |
| Q5120 | ||
The follow codes have age restrictions:
- J1201 – 6 months and older
- J1558 – 2 years and older
- J0791 – 16 years and older
- J0223, J0691, J0742, J0896, J7169, J9177, J9246, J9358, Q5119, Q5120 – 18 years and older
The following codes are diagnosis restricted:
- J0223 for Injection, givosiran, 0.5 mg (Givlaari)
- Restricted to diagnosis codes E8020, E8021, and E8029
- Q5120 for Injection, pegfilgrastim-bmez, biosimilar, (ZIEXTENZO), 0.5 mg
- Diagnosis allowed for this code are located in the TMPPM, Clinician-Administered Drugs Handbook, subsection 22, “Colony Stimulating Factors (Filgrastim, Pegfilgrastim, and Sargramostim”
The following codes require prior authorization:
- Code J0791 for Injection, crizanlizumab-tmca, 5 mg (Adakveo) is replacing code C9053 and will follow the same prior authorization requirements.
The following codes can be billed with Modifier JW:
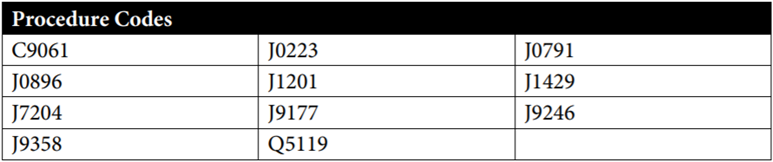
Effective March 1, 2020, code C9803 became a benefit and can be used for specimen collections for Coronavirus testing.
Update for September 10, 2020: TCHP will follow the guidance from HHSC and reprocess claims for procedure codes C9803 that were denied or that did not include the additional payment, waiving the 95-day filing deadline for providers that had not submitted claims. This is for the remainder of the disaster declaration period.
Resource:
Reimbursement Rate Updates for Procedure Code C9803 Effective March 1, 2020 for Medicaid, FPP, HTW, and the CSHCN Services Program
The following codes have been discontinued and should not be reimbursed after June 30, 2020:
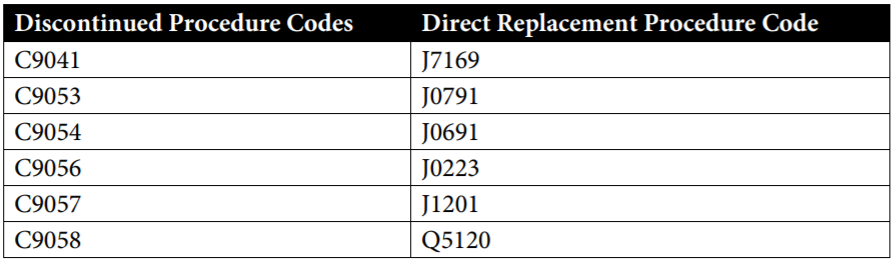

The following codes have been revised:

Next steps for providers: The provider notice is available on the TMHP website. Providers should ensure staff are aware of this guidance.
If you have any questions, please email Provider Network Management at: providerrelations@texaschildrens.org.
For access to all provider alerts, log into:
www.thecheckup.org or www.texaschildrenshealthplan.org/for-providers.





Leave a Reply
You must be logged in to post a comment.