Provider Alert! Medicaid Preferred Drug List and Formulary Changes
Date: July 30, 2021
Attention: All Providers
Effective Date: July 29, 2021
Providers should monitor the Texas Children’s Health Plan (TCHP) Provider Portal regularly for alerts and updates associated to the COVID-19 event. TCHP reserves the right to update and/or change this information without prior notice due to the evolving nature of the COVID-19 event.
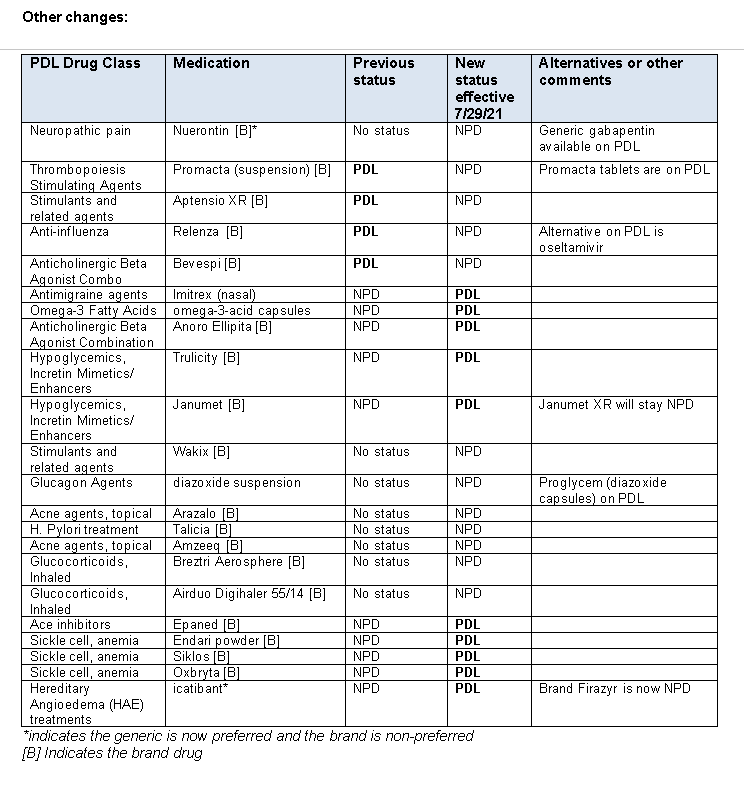
Call to action: The Texas Vendor Drug Program (VDP) implemented changes to the state Medicaid drug formulary, effective Thursday, July 29, 2021. Select medications moved from “preferred” to “non-preferred” status and vice-versa. Texas Children’s Health Plan wanted to notify providers so that these changes do not impact the ability of your STAR and STAR Kids members to obtain their medications. A summary of the changes is included below.
Resources: https://www.txvendordrug.com/about/news/2021/july-2021-preferred-drug-list-now-available.

How this impacts providers: Preferred and non-preferred medications may continue to require clinical prior authorizations. In addition to any clinical prior authorization requirements, non-preferred medications will also require a “step therapy prior authorization.” This means that STAR and STAR Kids members must have attempted and failed at least one preferred medication before obtaining a non-preferred medication. The preferred drug list (PDL) can be found on the VDP website (link below). Medicaid managed care plans are required to follow the PDL.
Next steps for providers: Preferred drugs are medications recommended by the Texas Drug Utilization Review Board for their efficaciousness, clinical significance, cost effectiveness, and safety. Texas Children’s Health Plan encourages providers to initiate a preferred medication to members new to therapy. When possible, Texas Children’s Health Plan also encourages switching existing members to a preferred agent.
If you have any questions, please email Provider Network Management at: tchppharmacy@texaschildrens.org.
For access to all provider alerts, log into:
www.thecheckup.org or www.texaschildrenshealthplan.org/for-providers.
Resources:
https://www.txvendordrug.com/formulary/prior-authorization/preferred-drugs.







Leave a Reply
You must be logged in to post a comment.